
Bed bath in patients with acute coronary syndrome: algorithm description
Viviane de Moraes Sptiz1, Lucelia Santos2, Fernanda Reis3, Aretha Pereira de Oliveira4, Monyque Evelyn dos Santos Silva5, Dalmo Machado6
1 Secretaria Estadual de Saúde do Estado do Rio de Janeiro
2 Secretaria Municipal de Saúde do Rio de Janeiro
3 Hospital Estadual Alberto Torres
4 Instituto Nacional do Câncer
5 Universidade Veiga de Almeida
6 Universidade Federal Fluminense
ABSTRACT
Aim: to build an algorithm for systematization of traditional bed bath steps in an adult patient with acute coronary syndrome. Method: this is a descriptive study designed in line with the integrated project “Myocardial oxygen uptake and hemodynamic aspects during bed bath in patients with acute myocardial infarction”. The algorithm was built by Bizagi Modeler version 3.0. Results: The algorithm was broken into two parts: evaluation and decision making about the temperature of the water to be used in the bath and the execution of the bath. The latter was divided into three subparts: dorsal, lateral and finishing hygiene, with specific execution times. Conclusion: the algorithm was an innovative project and can be used both in care practice and as an educational tool. The next step will be validation by experts.
Descriptors: Algorithms; Baths; Acute Coronary Syndrome.
INTRODUCTION
Algorithms have often been used in health services as a way to systematize care and management practices. Its main objective is to direct decision making(1). Its use enables greater security, risk reduction, time optimization and cost reduction. With this, these tools provide a safe and oriented care practice in various areas of health, including nursing, not removing the ability to think, but leading the evaluator and performer to a direction related to the care provided(1).
Risk classification in emergencies and emergency services are good examples of the applicability of the algorithm in the health service. The use of a colorful algorithm designed to direct care in order of priority decreases the outcomes of the patient's clinical condition and even death(2).
In the national and international scientific literature, no record of any algorithm on bed bath in patients with acute coronary syndrome (ACS) has been found. However, there are protocols and flow charts of criteria for bed bath indication in intensive care unit (ICU) patients(3) and for bed bath anxiety reduction(4), but none of them consider the patient's oxyhemodynamic state.
Based on previous studies carried out in critically ill patients and demonstrating that bed bathing can have repercussions on oxygenation and body perfusion dynamics(5, 6, 7), the objective of this study was to construct an algorithm for the systematization of traditional bed bath steps in adult patients with ACS.
METHOD
Descriptive study conducted from 2015 to 2017 as part of the professional master's program of the Fluminense Federal University, with the collaboration of the Cardiovision Research Center, composed of nurses and nursing academics.
This study was part of a strand of the integrated project “Myocardial oxygen uptake and hemodynamic aspects during bed bath in patients with acute myocardial infarction”, whose objectives were: to investigate the hemodynamic and myocardial oxygen uptake repercussions during postural change in the supine, left and right lateral decubitus; to compare hemodynamic and myocardial oxygen consumption repercussions during bed bath, under temperature and positioning control, in patients with acute myocardial infarction and not infarcted; and to construct an algorithm for the indication of bathing in hospitalized adult patients, based on oxyhemodynamic repercussions.
Decision making on the best type of bath was systematically outlined, relating water temperature to myocardial oxygen consumption, guided by the initial hemodynamic evaluation in Killip-Kimball I and II patients with ACS(8).
The algorithm was structured on two pillars: the systematic description of bathing steps according to Potter and Perry(9) and the extraction and evaluation of data from the integrated project. Scientific literature data were also used to support the standard of normality of the variables extracted from the integrated project and the changes related to the bed bath, based on the systematic review entitled “Oxyhemodynamic bath repercussions in critically ill adult patients: evidence from systematic literature review(5).
The construction of the algorithm involved three phases: transcription and adaptation of the bed bath steps; extraction and analysis of integrated project data; and the algorithm construction itself.
Phase 1: transcription and adaptation of bathing steps
The transcription and adaptation of the bed bath steps described by Potter and Perry(9) were performed, according to the bath protocol that would be used for the construction of the algorithm. The adaptation of the bathing steps was directed to the current practice and focused on the bed bath of ACS patients admitted to the ICU. The key points of this adaptation are: verification of vital signs before the beginning of the bath and to direct the water temperature to be used; maintenance of patient monitoring during bed bath; covering the peripheral vascular access with plastic as a means of preventing primary bloodstream infection; washing of the genitalia in the supine position; non-use of bedpan to avoid extra effort; applying 70% alcohol on the mattress before covering it with a new sheet to reduce the bacterial load; replacement of electrodes; checking vital signs after bathing; and reprogramming the monitor alarms.
Phase 2: Integrated Project Data Collection
The findings of the integrated project “Myocardial oxygen consumption and hemodynamic aspects during bed bath in patients with acute myocardial infarction” were the other pillar of the algorithm. This was an uncontrolled randomized clinical trial designed with Killip-Kimbal I and II ACS patients admitted to the coronary care unit of a large private hospital in Niterói, RJ. The project was approved by the Research Ethics Committee of the Fluminense Federal University Medical School under Opinion No. 1285852, in June 2015, and inserted in the Brazilian Registry of Clinical Trials (RBR-555p8y) and the Universal Trial Number. (U1111-1174-0316).
The clinical trial consisted of two baths designated as experiment and control. The experiment bath was performed with a constant water temperature at 40°C(10), maintained by a heating plate and using a probe to measure the temperature. The control bath was performed with water taken directly from a heated tap, without maintaining the temperature constancy(11). The execution of the bed bath was also evaluated by two performers, and a maximum time of 20 minutes was set for the procedure(10,11).
The effect of bath water temperature on oxyhemodynamic variables was evaluated by transthoracic electrical bioimpedance (TEB). Data were extracted from bioimpedance and transferred to a spreadsheet. Statistical evaluation of the data was performed using the Statistical Package for Social Sciences for Windows (SPSS), version 21.0. Descriptive statistics used the mean and standard deviation. To test the difference in mean myocardial oxygen consumption (mVO2), the Student T hypothesis test for independent samples was adopted. It was considered a significance level (α) of 5% and a confidence interval of 95%.
The bioimpedance was calibrated to accurately provide the 79 measurements, and the entire research team was trained to handle the equipment and to standardize the execution of the bath steps. Data collection was performed from June 2015 to March 2016.
For the construction of the bed bath algorithm, the data collected from 19 ACS patients with and without ST-segment elevation and with Killip-Kimball I or II classification were used. The oxyhemodynamic variable chosen for the comparison base was mVO2 consumption, as it is a determinant in the preservation of the myocardial muscle(12). Using the Hellerstein and Wenger equation(13), mVO2 was determined by indirect calculation from the double product (DP), which results from the multiplication between systolic blood pressure (SBP) and heart rate (HR), according to the formula:
The other variables used in the construction were: HR, SBP, diastolic blood pressure (DBP), mean arterial pressure (MAP), systolic volume (SV) and peripheral arterial oxygen saturation (SaO2).
The purpose of the comparison between water temperature and oxyhemodynamic variables was to determine the best type of bath for each patient's hemodynamic condition prior to bathing. Patients were classified into groups according to the variables mentioned before, per and post-bath. The normal values of each variable were determined by the literature.
Water temperature had an effect on mVO2 in HR, SBP and MBP variables. The effect on HR occurred only in tachycardic patients (HR> 100 bpm) prior to the beginning of the bath. In these patients, bathing with spontaneous decrease in water temperature was the best option, since it did not significantly increase mVO2, in contrast to the constant temperature bed bath at 40°C, which promoted a statistically significant change (p=0.04).
In patients with SBP≥ 140 mmHg, bathing without constant water temperature significantly changed mVO2 (p=0.01). This did not happen when the water temperature remained constant at 40°C, making this bath more beneficial for the patient. The same was true for patients with normal MAP (93-106 mmHg) before bathing: a significant increase in mVO2 (p=0.01) was observed in the bath with a spontaneous decrease in water temperature. This patient therefore benefited most from the bath with constant water control at 40°C. On the other hand, patients with low MAP (≤ 83 mmHg) and whose bath was carried out with water at constant temperature at 40°C presented a significant increase in mVO2 (p=0.01), considering the best choice for bath without water temperature manipulation.
RESULTS
The algorithm
The algorithm was made using free software Bizagi Modeler version 3.0, which allows process modeling for decision making. The choice of this software is due to its ease of application and offers technical support with consultants to assist in the construction of the process.
From the statistical analysis of the results of the integrated project, it was evidenced that the bed bath should follow two paths differentiated by water temperature: (i) constant water temperature at 40°C when SBP ≥ 140 mmHg; (ii) and bath water without temperature constancy when HR ≥ 100bpm.
The steps were entered into the software manually and two paths were traced according to the variables. The cohort points for these findings were considered by the literature review of normativity of the variables described in the cardiology guidelines.
The process modeling performed by Bizagi Modeler version 3.0 is composed of geometric figures that have their own notation and for specific purposes (Figure 1).
Figure 1. Legend of Bizagi Geometric Figures. 2017, Niterói, Brazil(14).
FIGURE 1

Each geometric shape has meaning for decision making, as described below:
A. Pool: Rectangular shape that houses the contents of the process. The process name is entered in the rectangle header;
B. Lane: rectangles within the pool representing departments and areas that interconnect during the same process;
C. Task: Rounded rectangles that determine the tasks performed in the process;
D. Gateway or Decision: Diamond whose purpose is to control the decision making of an activity. These points can be divergent (when the floodgate points to two or more paths in the stream) or convergent (when two paths join in one in the stream);
E. Initial event: green circle;
F. Intermediate event: double circle;
G. Final event: red-colored circle, which means the end of the process;
H. Sequence connector: angled arrow used to link activities within the same process;
I. Message Connector: Dotted connector that expresses the connection between interconnecting process messages.
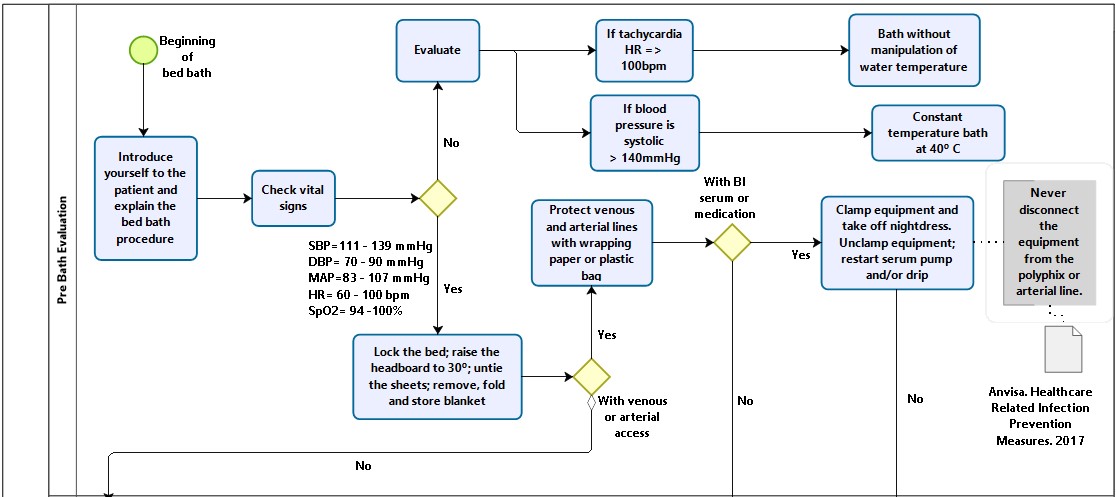
The elaboration of the algorithm was divided into four sessions or lanes. Lane 1 or first session was titled “Pre-Bath Assessment”. In this session it was determined that nurses should introduce themselves to the patients and introduce the team that will perform the bath, provide the necessary guidance on the bed bath, carefully evaluate the patient and their vital signs, decide on the type of bath with or without constant water temperature control, protect the vascular access with plastic, and undress the patient (Figure 2).
Figure 2. Pre-bath evaluation. 2017, Niterói, Brazil(14).
FIGURE 2
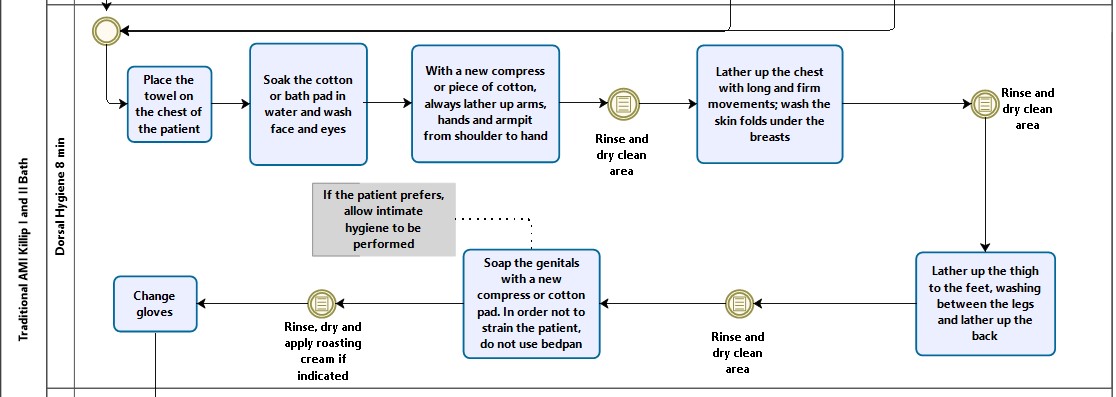
The second session or lane 2 was titled “Dorsal Hygiene 8 min”. It describes the bath performed in the supine position, including facial, eye, limb, chest and genital hygiene. This session demands more time from the performer, 8 minutes, as practically the entire body will be sanitized at this time, justifying the time determination in the subtitle (Figure 3).
Figure 3. Dorsal hygiene 8 min. 2017, Niterói, Brazil(14).
FIGURE 3
The third session or lane 3 was titled “Side Hygiene 6 min”. It describes the choice of the first lateralization, that is, to which position the patient will be lateralized for the dorsal region hygiene. At this time, care is given to the back and perianal region. It is a stage of the bath that allows the performer to observe the integrity of the skin and promote hydration and care with it.
Also at this stage will be the removal of wet and dirty clothes, the quick cleaning of the mattress with 70% alcohol and the lining of the bed with clean sheets, oiled and traces. It is noteworthy that different times were determined for right lateral decubitus (RLD) and left lateral decubitus (LLD). For LLD, a time of 2 minutes, considered a safety time for no oxyhemodynamic repercussions, was stipulated(10,11). For RLD, a time of four minutes was stipulated and this position should be the choice for performing back hygiene due to the longer time to perform the proposed care for this procedure.
The fourth session or lane 4 was called “Bathing time 6 min” and corresponds to the completion of the bath. It includes the following actions: dressing the patient, applying deodorant, moisturizer and rash cream, if indicated; change electrodes and reprogram monitors and alarms; remove the protections from the vascular lines, arrange the patient's bed, and discard the consumables used in the bath. Sessions 3 and 4 are presented in Figure 4.
Figure 4. Lanes 3 and 4: lateral hygiene and bath completion, respectively. 2017, Niterói, Brazil(14).
FIGURE 4
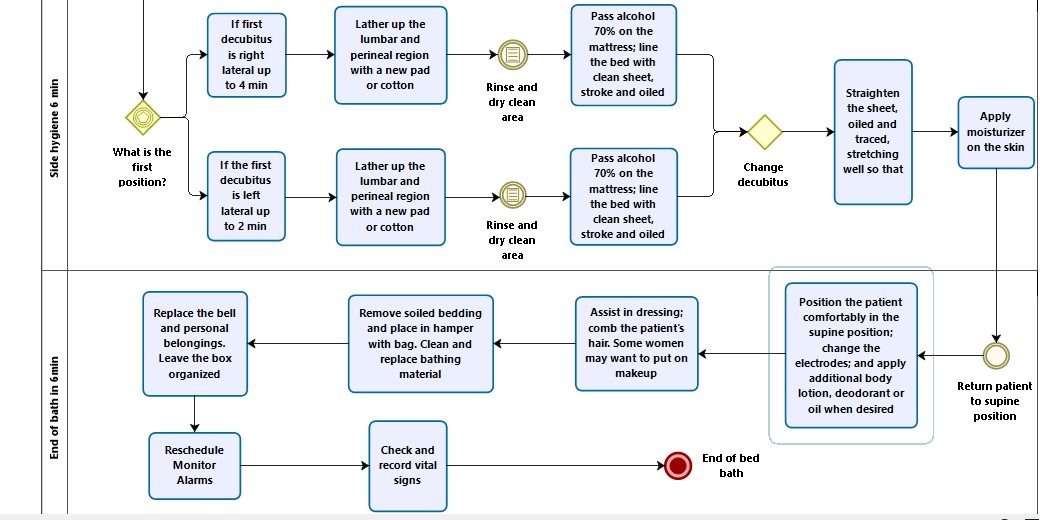
Figure 5 presents the bath algorithm in its entirety, in which it is possible to verify the steps taken.
Figure 5. Bathing algorithm in bed. 2017, Niterói, Brazil(14).
FIGURE 5

DISCUSSION
In an era where technology has been used to improve health quality, based on patient safety, there is a need to envision new tools for care practice. Algorithms, care flow charts, protocols, manuals, and guidelines are clinical tools that can ensure care that avoids or minimizes patient injury.
The decision model or algorithm is determined by a mathematical structure that recommends outcomes, fragmenting the problem into small parts, mapping the most relevant data, and relating initial and final data(15). As for the use of the algorithms, they can be presented in written or electronic format. The electronic format has the ability to expedite access to information, and improve communication and decision making(1,16). Some studies consider that algorithms or other graphical tools, preceded by figures for decision making, have positive points and effectiveness in decision making(1).
In this sense, the search for excellence in care quality delivered to the population has focused on the creation of algorithms directed to decision making in specific situations, which aim to minimize the risks arising from care practices. These include the National Patient Safety Program and safe practice guidance manuals.
Other algorithmic records for evaluation and decision making can be found in the scientific literature. A randomized controlled trial of 321 patients on mechanical ventilation tested the use of a sedation algorithm applied by nurses and obtained a satisfactory response. This algorithm, aimed at sedation weaning, was intended to decrease the time spent on mechanical ventilation, the length of stay in the ICU and hospital, and the tracheostomy achievements(17). Another study investigated the feasibility, safety and efficacy of the nurse-applied glycemic control protocol called N-DIABIT. This protocol favored the management of hyperglycemia and control of hypoglycemic episodes by nurses, demonstrating efficacy and efficiency in this control(18).
However, there was a lack of knowledge and the absence of a specific tool for guidance or decision making about bed bath in patients with ACS. As evidenced by the integrated design, there may be even minimal oxyhemodynamic repercussions in patients under these conditions. These events can be prevented by careful patient assessment before bathing and a decision-making tool can direct an intervention without unpleasant outcomes.
Guidelines for ACS patient care require bed rest for at least 72 hours as a means of sparing the heart muscle(19). This is because ACS patients need to decrease myocardial oxygen consumption and energy expenditure, maintain heart rate and hemodynamic stability, and thus prevent further ischemic-related pain episodes(19).
It is noteworthy that in the integrated project, some precautions related to the assessment of vital signs before bed bathing and the maintenance of cardiac monitoring during bathing in patients with ACS were employed. It was observed that this care, employed in other research related to bed bath(4, 5, 6, 7), can foster the idea that nurses need to be more present in both initial assessment and bed bath. Nurses play a decisive role in making decisions in terms of how and when to perform bed bathing, as they are the holders of expertise on an exclusive nursing intervention and knowledge of the patient's clinical condition.
The use of tools such as the algorithm does not exempt nurses from careful patient assessment. The critical eye is something that needs to be in the essence of the professional, because like all technology it can have flaws. Likewise, in order to ensure the success of a tool, all the team that will use it needs to be trained in its application and evaluation of its results.
LIMITATIONS
A limitation of this study is the absence of evaluation of the outcome Heart Rate (HR), which is a variable described in some publications that evaluated the effect of bed bath(5,6). The Bioimpedance of CardioScreen used for the research did not include the measurement of this variable that could directly compromise the internal and external validity of the study, since the patient could interfere with the measurement and/or the researcher's counting could be flawed. As a way to have at least one variable that could portray oxygenation, SaO2 was used because it is able to predict cardiac dysfunction due to hypoxemia(20).
CONCLUSION
Considering that the use of robust tools guides the nursing practice, allowing safe care, the algorithm described was built with the intention of contributing to the nursing team in the evaluation of the patient with ACS in front of the bed bath and, thus, minimizing the occurrence of oxyhemodynamic changes during essential nursing intervention.
After its elaboration, it was observed that the tool can be used not only for quality care practice, but also as an educational instrument in basic nursing disciplines and even in continuing education processes. Its initial presentation was in written format, with the intention of turning it into an electronic tool. In addition, it can be used in public and private institutions, and can be adapted according to the bed bath materials and equipment available at the institution.
In order to improve the knowledge and improvement of care practice, new research on bed bath research and its effects should be developed to gain a better understanding of this nursing intervention. Other factors that may interfere with body oxyhemodynamic variables also need to be studied.
Thus, the next step to be developed will be the validation of the algorithm by experts, a relevant and essential step in the construction process, which will employ scientific and pedagogical value.
REFERENCES
Barra DCC, Dal Sasso GTM, Baccin CRA. Sistemas de alerta em um processo de enfermagem informatizado para Unidades de Terapia Intensiva. Rev. esc. enferm. USP [Internet], 2014 [cited 2018 Dec 02]; 48(1): 125-132. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0080-62342014000100125&lng=en. http://dx.doi.org/10.1590/S0080-623420140000100016.
Becker JB, Lopes MCBT, Pinto MF, Campanharo CRV, Barbosa DA, Batista REA. Triagem no Serviço de Emergência: associação entre as suas categorias e os desfechos do paciente. Rev Esc Enferm USP [Internet]. 2015 [cited 2017 Mar 20];49(5):783-9. Available from: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S008062342015000500783&lng=en. doi http://dx.doi.org/10.1590/S0080623420150000500011.
Flores GP. Critérios para banho no leito em Unidade de Terapia Intensiva adulto: construção de um protocolo assistencial.(Dissertação de Mestrado). Porto Alegre: Universidade do Vale do Rio dos Sinos [Internet]; 2016 [cited 2018 Dez 02]. Available from:http://www.repositorio.jesuita.org.br/bitstream/handle/UNISINOS/5279/GRAZIELA%20PEREIRA%20FLORES_.pdf?sequence=1&isAllowed=y
Lopes JL, Barbosa DA, Nogueira-Martins LA, Barros ALBL. Nursing guidance on bed baths to reduce anxiety. Rev Bras Enferm [Internet]. 2015 [cited 2018 dez 02];68(3):437-43.Available from: http://www.scielo.br/pdf/reben/v68n3/0034-7167-reben-68-03-0497.pdf
DOI: http://dx.doi.org/10.1590/0034-7167.2015680317i
Lima DVM. Repercussões oxi-hemodinâmicas do banho no paciente adulto internado em estado crítico: evidências pela revisão sistemática de literatura [tese]. São Paulo: Universidade de São Paulo; 2009.
Oliveira AP, Lima DVM. Evaluation of bedbath in critically ill patients: impact of water temperature on the pulse oximetry variation. Rev Esc Enferm USP [Internet]. 2010 [cited: 2016 jan 21];44(4):1034-40. Available from: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S008062342010000400026&lng=en. doi http://dx.doi.org/10.1590/S008062342010000400026
Madrid SQ, López CC, Otálvaro AFT, Padilla LMR. Alteraciones hemodinámicas del paciente crítico cardiovascular durante la realización del baño diário. Medicina U.P.B. [Internet]. 2012 [cited 2016 Jan 20];31(1):19-26 Available from: https://revistas.upb.edu.co/index.php/Medicina/article/view/987/886
Mello BHG, Oliveira GBF, Ramos RF, Lopes BBC, Barros CBS, Carvalho EO, et al . Validação da Classificação de Killip e Kimball e Mortalidade Tardia Após Infarto Agudo do Miocárdio. Arq. Bras. Cardiol. [Internet], 2014 [cited 2018 Nov 02]; 103( 2 ): 107-117. Available from: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0066-782X2014002000004&lng=en.
Potter P, Perry A. Fundamentos de enfermagem. 9 ed. Rio de Janeiro: Elsevier; 2010.
Silva MES. Padrão hemodinâmico não invasivo dos efeitos do banho no leito com temperatura da água constante em pacientes com infarto agudo do miocárdio [dissertação]. Niteroi: Universidade Federal Fluminense; 2015.
Reis FF. Padrão hemodinâmico não-invasivo durante o banho no leito sem controle hidrotérmico de pacientes com infarto agudo do miocárdio: ensaio clínico randomizado [dissertação]. Niterói: Universidade Federal Fluminense; Niterói.
Paiva L, Providência R, Barra S, Dinis P, Faustino A, C, Gonçalves L: Universal Definition of Myocardial Infarction: Clinical Insights. Cardiology [Internet], 2015 [cited 2018 Nov 02];131:13-21. Availablefrom:https://www.karger.com/Article/ FullText/371739# doi: 10.1159/000371739
Hellerstein HK, Wenger NK. Rehabilitation of the coronary patients. New York: John Willey and Sons; 1978.
Sptiz VM. Construção de um algoritmo baseado em evidências para o banho no leito em pacientes com síndrome coronariana aguda. Niterói Dissertação [Mestrado Profissional em Enfermagem]- Universidade Federal Fluminense, 2017.
Goiás. Secretaria de Estado de Gestão e Planejamento do Estado de Goiás. Modelagem de Processo com Bizagi Moedeler [Internet]. Goiânia: SEGPLAN; 2014 [cited 2016 Nov 22]. Available from: http://www.sgc.goias.gov.br/upload/arquivos/2014-10/manual-de-padronizacao-demodelagem-de-processos-usando-bizagi---v3-1.pdf
Segal G, Karniel E, Mahagna A, Kaa'dan F, Levi Z, Balik C. A nurse-guided, basal-prandial insulin treatment protocol for achieving glycaemic control of hospitalized, non-critically ill diabetes patients, is non-inferior to physician-guided therapy: A pivotal, nurse-empowerment study. Int J Nurs Pract [Internet] 2015 [cited 2017 Jan 29]21(6):790-6. Available from: https://onlinelibrary.wiley.com/doi/abs/10.1111/ijn.12292 doi: 10.1111/ijn.12292.
Brook AD, Ahrens TS, Schaiff R, Pretenci D, Sherman G, Shannon W, Kollef MH. Effect of a nursing-implemented sedation protocol on the duration of mechanical ventilation. Crit Care Med.1999 Dec.;27(12):2609-15.
Manders IG, Stoecklein K, Lubach CHC, Bijl-Oeldrich J,Nanayakkara PWB,Rauwerda JA, et al. Shiftin responsibilities in diabetes care: the Nurse-Driven Diabetes In-Hospital Treatment protocol (N-DIABIT). Diabetic Med [Internet]. 2016 [cited 2017 mar 20];33(6):761-767. Available from: http://onlinelibrary-wiley-com.ez24.periodicos.capes.gov.br/doi/10.1111/dme.12899/epdf DOI:10.1111/dme.12899
Piegas LS, Timerman A, Feitosa GS, Nicolau JC, Mattos LAP, Andrade MD et al. V Diretriz da Sociedade Brasileira de Cardiologia sobre Tratamento do Infarto Agudo do Miocárdio com Supradesnível do Segmento ST. Arq. Bras. Cardiol. [Internet]. 2015 [cited 2016 Nov 27];05(2 Suppl I):1-121. Available from: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0066782X2015003000001&lng=en. doi http://dx.doi.org/10.5935/abc.20150107
Stub D, Smith K, Bernard S, Nehme Z, Stephenson M, Bray JE, et al. Air Versus Oxygen in ST-Segment Elevation Myocardial Infarction. Circulation [Internet], 2015 [cited 2016 Jul 16];131:2143-50. Available from:https://doi.org/10.1161/CIRCULATIONAHA.114.014494
All authors participated in the phases of this publication in one or more of the following steps, in according to the recommendations of the International Committee of Medical Journal Editors (ICMJE, 2013): (a) substantial involvement in the planning or preparation of the manuscript or in the collection, analysis or interpretation of data; (b) preparation of the manuscript or conducting critical revision of intellectual content; (c) approval of the version submitted of this manuscript. All authors declare for the appropriate purposes that the responsibilities related to all aspects of the manuscript submitted to OBJN are yours. They ensure that issues related to the accuracy or integrity of any part of the article were properly investigated and resolved. Therefore, they exempt the OBJN of any participation whatsoever in any imbroglios concerning the content under consideration. All authors declare that they have no conflict of interest of financial or personal nature concerning this manuscript which may influence the writing and/or interpretation of the findings. This statement has been digitally signed by all authors as recommended by the ICMJE, whose model is available in http://www.objnursing.uff.br/normas/DUDE_eng_13-06-2013.pdf
Reviewed:2019/04/08
Approved:2019/04/08